Port Neches, TX (409) 727-1122

Treatment Options for Sweaty Feet
People who have feet that sweat excessively may have a condition that is known as plantar hyperhidrosis. It may be the result of a neurological or endocrine disorder and can be quite uncomfortable. There are several treatment options, and this can depend on the severity of this ailment. Surgery may be a viable option for successfully removing the sweat glands. Patients who are afflicted with this condition often keep an extra pair of shoes and socks close by. It can be professionally and socially disabling, and many patients who have this condition are often embarrassed. If you think you may have hyperhidrosis, it is suggested that you schedule an appointment with a podiatrist who can offer you the correct treatment solutions.
If you are suffering from hyperhidrosis contact Pete O’Donald, DPM of Texas. Our doctor can provide the care you need to attend to all of your foot and ankle needs.
Hyperhidrosis of the Feet
Hyperhidrosis is a rare disorder that can cause people to have excessive sweating of their feet. This can usually occur all on its own without rigorous activity involved. People who suffer from hyperhidrosis may also experience sweaty palms.
Although it is said that sweating is a healthy process meant to cool down the body temperature and to maintain a proper internal temperature, hyperhidrosis may prove to be a huge hindrance on a person’s everyday life.
Plantar hyperhidrosis is considered to be the main form of hyperhidrosis. Secondary hyperhidrosis can refer to sweating that occurs in areas other than the feet or hands and armpits. Often this may be a sign of it being related to another medical condition such as menopause, hyperthyroidism and even Parkinson’s disease.
In order to alleviate this condition, it is important to see your doctor so that they may prescribe the necessary medications so that you can begin to live a normal life again. If this is left untreated, it is said that it will persist throughout an individual’s life.
A last resort approach would be surgery, but it is best to speak with your doctor to find out what may be the best treatment for you.
If you have any questions please feel free to contact our office located in Nederland, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Hyperhidrosis of the Feet
Hyperhidrosis of the feet, also termed plantar hyperhidrosis, is characterized by excessive sweating of the feet that can be onset by any cause, such as exercise, fever, or anxiety. Most people suffering from hyperhidrosis of the feet also experience hyperhidrosis of the hands, or palmar hyperhidrosis. Approximately 1-2% of Americans suffer from this disorder.
Sweating is a healthy process utilized by the body in order to cool itself and maintain a proper internal temperature, which is controlled by the sympathetic nervous system. In individuals with hyperhidrosis, the sympathetic nervous system works in "overdrive", producing far more sweat than is actually needed.
Plantar hyperhidrosis is considered primary hyperhidrosis. Secondary hyperhidrosis refers to excessive sweating that occurs in an area other than the feet, hands, or armpits, and this indicates that is related to another medical condition, such as menopause, hyperthyroidism, or Parkinson's disease.
Symptoms of hyperhidrosis of the feet can include foot odor, athlete's foot, infections, and blisters. Because of the continual moisture, shoes and socks can rot which creates an additional foul odor and can ruin the material, requiring shoes and socks to be replaced frequently. In addition to the physical symptoms, emotional health is often affected as this disorder can be very embarrassing.
If left untreated, hyperhidrosis will usually persist throughout an individual's life. However, there are several treatment options available. A common first approach to treating hyperhidrosis of the feet is a topical ointment. Aluminum chloride, an ingredient found in antiperspirants, can be effective at treating hyperhidrosis if used in high concentration and applied to the foot daily. Some individuals can experience relief this way, while others encounter extreme irritation and are unable to use the product. Another procedure is the use of Botulinum Toxin A, commonly referred to as Botox. This is injected directly into the foot, and is effective at minimizing the sweat glands in the injected area. These injections must be repeated every 4 to 9 months.
If these treatments are ineffective, oral prescription medications may be taken in an effort to alleviate the symptoms. Again, some will experience relief while others do not. Going barefoot reportedly provides relief for most sufferers.
A final approach to combating hyperhidrosis of the feet is through surgery. Surgery has been less successful on patients with plantar hyperhidrosis than on those with palmar hyperhidrosis. It is only recommended when sweating is severe and other treatments have failed to work. This kind of surgery usually involves going into the central nervous system, and cutting nerves to stop the transmission of signals telling the foot to sweat.
Types of Arthritis That Can Affect Your Feet
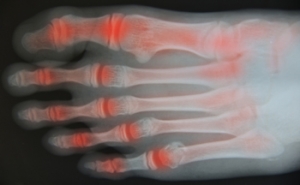
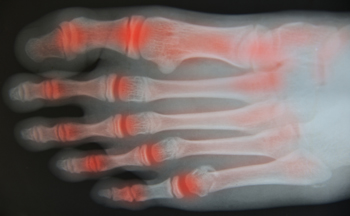
The feet and ankles contain numerous joints that can be affected by several types of arthritis. Osteoarthritis, which has been called “wear and tear” on the joints, can develop slowly and worsen over time. It is caused by the deterioration of the cartilage that sits between the bones and can cause stiffness, pain, loss of flexibility, bone spurs and swelling. Inflammatory arthritis, of which there are several varieties, causes pain, swelling, redness, and/or heat around the joint. The most common form of arthritis is rheumatoid arthritis which is an autoimmune condition that attacks healthy cells and can cause long-term damage to the foot and ankle joints. Psoriatic arthritis is an overreaction of the immune system and can contribute to plantar fasciitis and Achilles tendinopathy, both extremely painful conditions. Another type of arthritis, one that usually attacks the big toe, is commonly called gout. It is caused by crystals that form inside the joint, producing extreme pain, swelling and redness. If left untreated it could lead to osteoarthritis. If you are experiencing any of these symptoms, it is a good idea to consult a podiatrist for a full diagnosis and options for treatment.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Pete O’Donald, DPM from Texas. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions, please feel free to contact our office located in Nederland, TX . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Arthritic Foot Care
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.
What Are Heel Spurs?
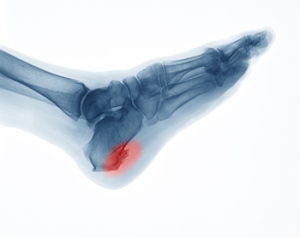
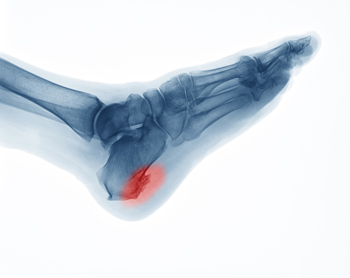 Heel spurs, or “enthesophytes,” develop on the heel of the foot. There are two types of heel spurs associated with different heel problems. One type of heel spur is called a Plantar Spur. It is linked to a problem called “Heel Spur Syndrome” and is a bone spur that develops on the bottom of the heel, on the sole of the foot where the plantar fascia (a band of fibrous tissue that stretches along the bottom of the foot) connects to the heel bone. People who have plantar fasciitis are prone to developing these kinds of spurs, which are the bone’s response to stress from straining foot muscles and ligaments, overstretching the plantar fascia, or repeated tearing of the thin lining of the heel bone. They are also associated with age, obesity, and osteoarthritis. Heel spurs are less likely to feel painful. The other type of heel spur is a Dorsal Spur and is connected to a problem called “Insertional Achilles Tendonitis,” a condition where a bone spur develops at the back of the heel, where the Achilles tendon fits into the bone. If you notice a bony protrusion on the heel of your foot or have pain in this area, it is best to consult with a podiatrist who can diagnose the problem and recommend proper treatment.
Heel spurs, or “enthesophytes,” develop on the heel of the foot. There are two types of heel spurs associated with different heel problems. One type of heel spur is called a Plantar Spur. It is linked to a problem called “Heel Spur Syndrome” and is a bone spur that develops on the bottom of the heel, on the sole of the foot where the plantar fascia (a band of fibrous tissue that stretches along the bottom of the foot) connects to the heel bone. People who have plantar fasciitis are prone to developing these kinds of spurs, which are the bone’s response to stress from straining foot muscles and ligaments, overstretching the plantar fascia, or repeated tearing of the thin lining of the heel bone. They are also associated with age, obesity, and osteoarthritis. Heel spurs are less likely to feel painful. The other type of heel spur is a Dorsal Spur and is connected to a problem called “Insertional Achilles Tendonitis,” a condition where a bone spur develops at the back of the heel, where the Achilles tendon fits into the bone. If you notice a bony protrusion on the heel of your foot or have pain in this area, it is best to consult with a podiatrist who can diagnose the problem and recommend proper treatment.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Pete O’Donald, DPM from Texas. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Nederland, TX . We offer the latest in diagnostic and treatment technology to meet your needs.
Heel Spurs
Heel spurs are the result of calcium deposits that cause bony protrusions on the underside of the heel. Heel spurs are usually painless, but they have the potential to cause heel pain. Heel spurs tend to be associated with plantar fasciitis, which is a condition that causes inflammation of the band of connective tissue that runs along the bottom of the foot. They most often occur to athletes whose sports involve a lot of running and jumping.
Some risk factors for developing heel spurs include running and jogging on hard surfaces, being obese, wearing poorly fitting shoes, or having walking gait abnormalities.
It is possible to have a heel spur without showing signs of any symptoms. However, if inflammation develops at the point of the spur’s formation, you may have pain while walking or running. In terms of diagnosis, sometimes all a doctor needs to know is that the patient is experiencing a sharp pain localized to the heel to diagnose a heel spur. Other times, an x-ray may be needed to confirm the presence of a heel spur.
Heel spurs can be prevented by wearing well-fitting shoes that have shock-absorbent soles. You should also be sure that you are choosing the right shoe for the activity you want to partake in; for example, do not wear walking shoes when you want to go on a run. Additionally, maintaining a healthy weight can be beneficial toward preventing heel spurs, as it will prevent an excess amount of pressure being placed on the ligaments.
There are a variety of treatment options for people with heel spurs. Some of these include stretching exercises, physical therapy, shoe inserts, or taping and strapping to rest stressed muscles and tendons. If you have heel pain that lasts longer than a month, don’t hesitate to seek help from a podiatrist. Your doctor can help you determine which treatment option is best for you.
What Is Peripheral Neuropathy?
 The most common form of peripheral neuropathy affects the feet. When there is a problem affecting the nerves in the feet, one can experience tingling and numbness in the feet, shooting, stabbing, or burning pain there, loss of coordination and balance, and muscle weakness. There is typically an underlying condition for those with this disorder. Those with diabetes and the elderly are most apt to be affected by this condition. Loss of sensation and possible injury to the feet without knowing it is a dangerous combination. It is vital that one who suffers from this type of neuropathy takes proper and daily care of one’s feet. Such care includes keeping feet clean, looking for ingrown toenails, sores or signs of injury, moisturizing feet, and wearing proper fitting shoes. While symptoms can be intermittent, because of the danger involved and the progressive nature of the condition, it is suggested that one consult a podiatrist as early as possible for relief of symptoms and treatment recommendations.
The most common form of peripheral neuropathy affects the feet. When there is a problem affecting the nerves in the feet, one can experience tingling and numbness in the feet, shooting, stabbing, or burning pain there, loss of coordination and balance, and muscle weakness. There is typically an underlying condition for those with this disorder. Those with diabetes and the elderly are most apt to be affected by this condition. Loss of sensation and possible injury to the feet without knowing it is a dangerous combination. It is vital that one who suffers from this type of neuropathy takes proper and daily care of one’s feet. Such care includes keeping feet clean, looking for ingrown toenails, sores or signs of injury, moisturizing feet, and wearing proper fitting shoes. While symptoms can be intermittent, because of the danger involved and the progressive nature of the condition, it is suggested that one consult a podiatrist as early as possible for relief of symptoms and treatment recommendations.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with Pete O’Donald, DPM from Texas. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in Nederland, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Neuropathy
Neuropathy is the weakness, numbness, and pain in the hands and feet due to damage to the peripheral nerves. The peripheral nerves are responsible for sending information from the brain and spinal cord to the rest of your body. Causes of Neuropathy include: traumatic injuries, infections, metabolic problems, exposure to toxins, and diabetes.
Diabetes is the most common cause, with more than half of the diabetic population developing some type of neuropathy. There are several types of neuropathy and they vary based on the damage of the nerves. Mononeuropathy is classified as only one nerve being damaged. When multiple nerves are affected, it is referred as polyneuropathy. One of the types of polyneuropathy is distal symmetric polyneuropathy. It is the most common for people with diabetes and starts when the nerves furthest away from the central nervous begin to malfunction. The symptoms begin with pain and numbness in the feet and then they travel up to the legs. A rarer form of polyneuropathy is acute symmetrical peripheral neuropathy, which is a severe type that affects nerves throughout the body and is highly associated with Guillain-Barre syndrome, an autoimmune disorder that attacks the peripheral nervous system and can be fatal. Although there are many types of neuropathy, most of them share the same symptoms such as pain, extreme sensitivity to touch, lack of coordination, muscle weakness, dizziness, and digestive problems. Since neuropathy affects the nerves, those affected should be careful of burns, infection and falling, as depleted sensations disguise such ailments.
The best way to prevent neuropathy is to manage any medical conditions such as diabetes, alcoholism, or rheumatoid arthritis. Creating and managing a healthy lifestyle can also go a long way. Having a healthy diet full of fruits, vegetables, whole grains and lean protein can keep the nerves healthy. These types of food have the nutrients to prevent neuropathy. Regularly exercising can help as well, but it is best to consult with a doctor about the right amount. In addition to diet and exercise, avoiding risk factors will also prevent neuropathy. This includes repetitive motions, cramped positions, exposure to toxic chemicals, smoking and overindulging on alcohol.
Why Are My Feet Changing Color?
If you have noticed that your feet or toes turn white, and then change to blue or red and become painful, you may have a condition known as Raynaud’s phenomenon. It is usually caused by a change in temperature, but it can also be caused by stress. It is common in young people, and it affects more women than men. If symptoms start over the age of 40, it may indicate other underlying conditions, such as rheumatoid arthritis, auto-immune disease, or poor blood circulation. You may also experience symptoms such as pain, pins and needles, swelling, and stiffness in the joints that can last as little as a few minutes or as long as a few hours. Common precautions that may be taken include keeping your feet warm during cold weather, as well as avoiding smoking and caffeinated beverages, which both decrease circulation. If Raynaud's symptoms worsen enough to interfere with your daily life, it is suggested that you make an appointment with a podiatrist for a full exam and options for other treatments.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Pete O’Donald, DPM of Texas. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
- Muscle pain, stiffness, or weakness
- Numbness or cramping in the legs
- Skin discoloration
- Slower nail & hair growth
- Erectile dysfunction
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our office located in Nederland, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.